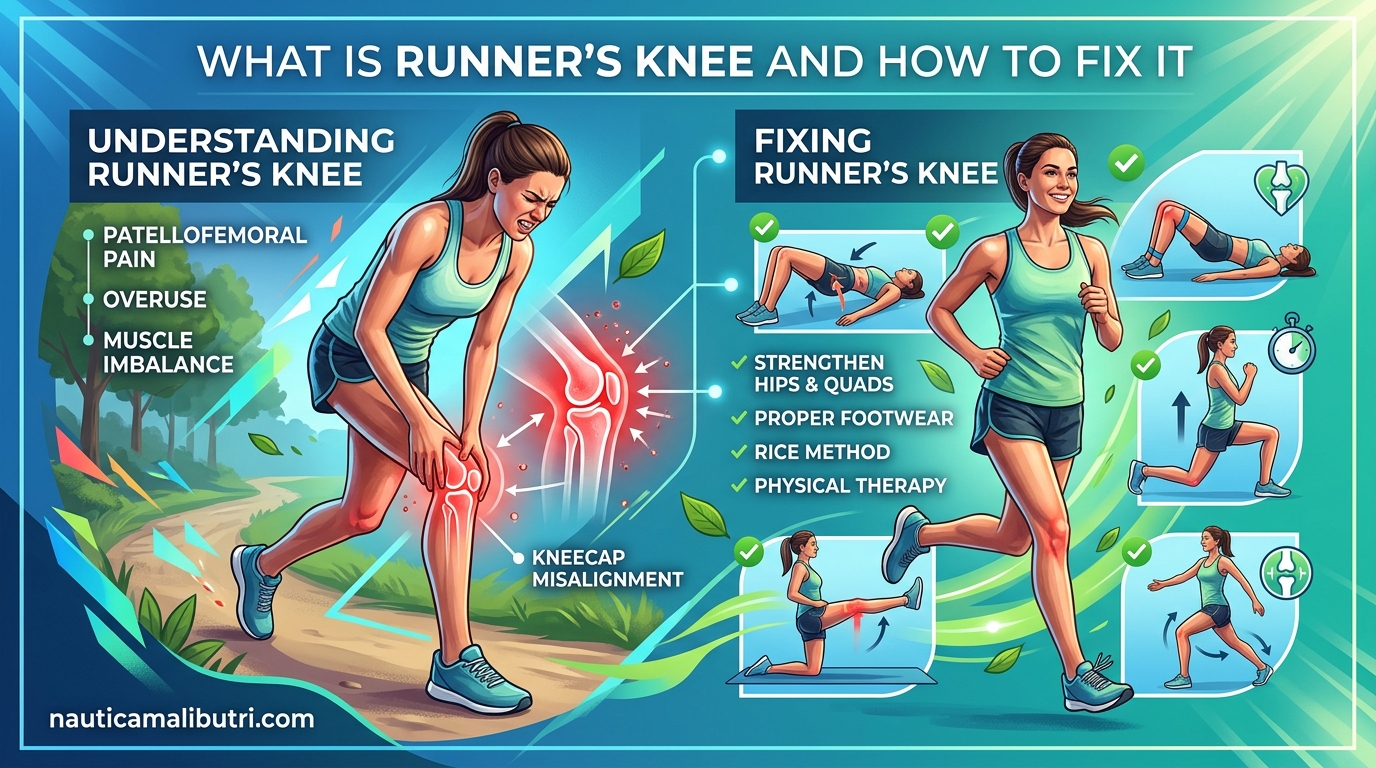
That sharp ache around your kneecap that shows up mid-run and lingers through the rest of your day is something most endurance athletes know too well. Runner’s knee affects up to 25% of runners and triathletes at some point in their training, making it one of the most common overuse injuries in multisport. I have worked with dozens of athletes who have faced this challenge during peak training blocks, and the good news is that it is both treatable and preventable with the right approach.
This guide covers everything you need to know about what is runner’s knee and how to fix it. You will learn the medical explanation behind patellofemoral pain syndrome, recognize the warning signs early, and follow a proven recovery protocol that gets you back to swimming, cycling, and running without surgery. Whether you are training for your first sprint triathlon or preparing for an Ironman, this article gives you the tools to manage knee pain and keep your training on track.
Table of Contents
What is Runner’s Knee?
Runner’s knee, medically known as patellofemoral pain syndrome (PFPS), is a condition that causes pain around or behind the kneecap. The patella (kneecap) normally glides smoothly in a groove at the end of your femur (thigh bone) called the trochlear groove. When this tracking becomes impaired, the cartilage beneath the patella experiences irritation and inflammation, leading to the characteristic pain that defines this condition.
The term “runner’s knee” is somewhat misleading because this injury affects more than just runners. Triathletes, cyclists, basketball players, and anyone who performs repetitive knee-bending activities can develop PFPS. The condition accounts for nearly 25% of all running-related injuries and represents one of the most frequent complaints sports medicine physicians see in their clinics.
Runner’s knee differs from other common knee injuries in several important ways. Unlike a meniscus tear, which often causes locking or catching sensations, PFPS creates a diffuse ache without mechanical symptoms. It is also distinct from iliotibial band syndrome, which typically produces pain on the outside of the knee rather than the front. Understanding these differences helps ensure you are treating the right condition.
Runner’s Knee Symptoms
Recognizing the specific symptoms of runner’s knee early can prevent a minor irritation from becoming a chronic training interruption. The pain typically develops gradually rather than following a specific traumatic incident. Most athletes describe the sensation as a dull, aching pain that localizes around or directly behind the kneecap.
The hallmark symptoms of patellofemoral pain syndrome include:
- Pain during activities that load the knee while bent, such as running downhill, descending stairs, or performing squats
- Aching sensation after prolonged sitting with knees bent, known as the “theater sign” because it affects people in movie theaters or at desks
- Discomfort when standing up after sitting for extended periods
- Pain that increases with activity duration and intensity
- Occasional grinding or clicking sensation beneath the kneecap during movement
- Swelling around the front of the knee in more severe cases
- Tenderness when pressing on the kneecap edges
For triathletes specifically, the pain often intensifies during the transition from bike to run. The cycling position keeps the knee in sustained flexion, and then the sudden impact of running creates a perfect storm for patellofemoral irritation. Many athletes report that their knee feels fine during the swim and bike portions but flares immediately when they start the run leg.
What Causes Runner’s Knee?
Understanding what triggers runner’s knee is essential for both treatment and prevention. The condition rarely has a single cause. Instead, it typically results from a combination of training errors, biomechanical factors, and muscle imbalances that create excessive stress on the patellofemoral joint.
Training and Overuse Factors
The most common trigger is sudden increases in training volume or intensity. Many triathletes fall into the trap of ramping up their running mileage too quickly while also adding bike intervals and swim sessions. This overloads the knee’s capacity to recover between workouts.
Downhill running creates particularly high patellofemoral stress because the knee stays bent longer during each stride while absorbing impact forces. Triathletes who train on hilly courses or perform lots of treadmill decline work are especially vulnerable. The same principle applies to stairs and step-down exercises.
Muscle Imbalances and Weakness
Weak hip abductors and external rotators are strongly linked to runner’s knee. When these muscles fail to stabilize the pelvis during single-leg stance, the thigh rotates inward excessively. This causes the patella to track laterally in its groove, increasing pressure on the outer cartilage surfaces.
The quadriceps also play a critical role. Weakness in the vastus medialis oblique (VMO), the inner portion of your front thigh muscle, allows the patella to pull toward the outside of the knee during extension. This malalignment creates the friction and irritation that leads to pain.
Biomechanical Issues
Foot mechanics significantly influence knee tracking. Overpronation, where the foot rolls inward excessively after landing, creates a chain reaction up the leg that stresses the patellofemoral joint. High arches can be equally problematic by limiting natural shock absorption and transferring more force to the knee.
Structural factors like knock knees (genu valgum), wide hips relative to ankle position (Q-angle), and leg length discrepancies can predispose certain athletes to PFPS. While you cannot change your bone structure, you can address the muscular and training factors that compound these biomechanical challenges.
Triathlon-Specific Causes
Triathletes face unique risk factors that pure runners do not encounter. Poor bike fit is a major contributor. A saddle that is too low or too far forward forces the knee into excessive flexion throughout the pedal stroke. This sustained compression of the patellofemoral joint, combined with the repetitive nature of cycling, creates significant irritation before you even start the run.
The transition run, or brick workout, presents another challenge. Coming off the bike, your legs are fatigued and your running mechanics are compromised. The initial miles of the run leg often involve a heavier foot strike and altered stride length that increases knee loading. Many triathletes report that their runner’s knee symptoms appear or worsen specifically during this transition phase.
How is Runner’s Knee Diagnosed?
Diagnosing runner’s knee typically starts with a thorough physical examination rather than immediate imaging. A healthcare provider will review your training history, symptom patterns, and any recent changes in activity or equipment. They will perform specific tests to reproduce your pain and rule out other conditions.
The physical exam usually includes palpation of the patella edges, compression tests that load the patellofemoral joint, and observation of your gait and single-leg squat mechanics. Your provider may check for quadriceps atrophy, assess hip strength, and evaluate your foot mechanics during walking and running.
Imaging studies are not always necessary for straightforward cases. X-rays primarily show bone and will not reveal the soft tissue irritation that characterizes PFPS. MRI can detect cartilage changes and rule out meniscus tears or ligament injuries, but it is usually reserved for cases that do not respond to initial treatment or when the diagnosis is unclear.
For self-assessment, consider whether your pain matches the classic PFPS pattern. Does it worsen with stairs, downhill walking, or after sitting? Is the pain diffuse around the kneecap rather than sharply localized? Does it improve when you stop the aggravating activity? Answering yes to these questions suggests runner’s knee, though professional evaluation is still recommended for confirmation.
How to Fix Runner’s Knee
Treating runner’s knee requires a multi-faceted approach that addresses both symptom management and underlying causes. The most effective protocols combine immediate care to reduce pain, targeted exercises to correct imbalances, and training modifications that allow healing while maintaining fitness. Here is the comprehensive treatment framework that has helped thousands of athletes return to full training.
Immediate Care: The RICE Protocol
The RICE protocol (Rest, Ice, Compression, Elevation) forms the foundation of acute runner’s knee management. This approach reduces inflammation, controls pain, and creates the conditions your knee needs to begin healing.
Rest does not necessarily mean complete inactivity. It means stopping the specific movements that aggravate your pain. For most triathletes, this involves cutting out running temporarily while maintaining swimming and possibly modifying cycling. Cross-training with non-weight bearing activities keeps your cardiovascular fitness intact while the knee recovers.
Ice therapy provides immediate pain relief and reduces inflammation. Apply ice packs or cold therapy systems to the front of your knee for 15-20 minutes at a time, several times daily. Many athletes ice after any activity that stresses the knee and again before bed. Use a thin towel between ice and skin to prevent frostbite.
Compression helps control swelling and provides proprioceptive feedback that may reduce pain. A simple elastic knee sleeve or patellar strap worn during daily activities can make a noticeable difference. The compression should be snug but not so tight that it causes numbness or tingling below the knee.
Elevation uses gravity to reduce fluid accumulation in the knee. When resting at home, prop your leg up so the knee sits above heart level. This is especially helpful in the evening after a day of activity. Combine elevation with icing for maximum effect.
Pain Management Options
Over-the-counter anti-inflammatory medications can help manage pain during the initial recovery phase. Ibuprofen, naproxen, or aspirin taken as directed reduce both discomfort and inflammation. These NSAIDs work best when combined with the rest and ice components of RICE rather than used alone to mask pain while continuing aggravating activities.
Topical anti-inflammatory gels containing diclofenac or similar compounds offer an alternative for those who prefer to avoid oral medications. Applied directly to the painful area, these products deliver medication locally with reduced systemic effects. Many athletes find them particularly helpful before bed.
Natural anti-inflammatory options include turmeric supplements, omega-3 fatty acids, and tart cherry juice. While the evidence for these is less robust than for NSAIDs, some athletes report benefit and they carry fewer side effect risks. These work best as adjuncts to the primary treatment protocol rather than replacements.
Supportive Measures: Braces, Taping, and Orthotics
Patellar straps and knee braces can provide symptomatic relief during activity. A patellar strap worn just below the kneecap changes the distribution of forces across the patellofemoral joint and may reduce pain during running or cycling. These are particularly useful during the return-to-activity phase.
Kinesiology taping (KT tape) and traditional athletic taping techniques can help with patellar tracking and proprioception. When applied correctly, tape gently pulls the patella into better alignment within its groove. Working with a physical therapist to learn proper taping technique ensures you get maximum benefit.
Custom or over-the-counter orthotics may help if biomechanical foot issues contribute to your runner’s knee. Arch supports that correct overpronation can improve lower extremity alignment and reduce the rotational forces that stress the patella. A gait analysis at a specialty running store can help determine if orthotics would benefit you.
Runner’s Knee Exercises for Recovery
Exercise-based rehabilitation is the cornerstone of lasting runner’s knee recovery. Strengthening the muscles that support proper patellar tracking while improving flexibility in tight tissues creates the biomechanical environment your knee needs to heal and stay healthy. The following protocol targets the specific weaknesses that contribute to PFPS.
Strengthening Exercises
Clamshells target the hip external rotators and abductors that stabilize your pelvis during running. Lie on your side with knees bent at 90 degrees and feet together. Keeping your feet touching, lift your top knee away from the bottom one like a clamshell opening. Hold for 2 seconds at the top, then lower slowly. Perform 3 sets of 15 repetitions per side.
Side-lying leg lifts strengthen the gluteus medius, a key muscle for preventing inward knee collapse. Lie on your side with the bottom knee bent for stability. Lift your top leg straight up about 12 inches, keeping the toe pointed forward rather than toward the ceiling. Do 3 sets of 15 repetitions per side, focusing on controlled movement.
Wall sits build quadriceps endurance without the patellofemoral stress of full squats. Stand with your back against a wall and slide down until your knees are bent at approximately 60-70 degrees. Hold this position for 30-60 seconds. Perform 3-5 repetitions. This angle strengthens the quads while minimizing joint compression.
Terminal knee extensions with a resistance band activate the VMO specifically. Sit with your leg extended and a band looped around a fixed point behind you. Bend your knee slightly, then straighten it completely while focusing on the final few degrees of extension. The VMO works hardest in this terminal range. Complete 3 sets of 20 repetitions.
Single-leg squats to a bench or box develop functional strength and stability. Stand in front of a bench set at knee height. Balance on one leg and lower yourself until you lightly touch the bench, then return to standing. Start with 2 sets of 8 repetitions per leg and progress gradually. Quality matters more than quantity.
Stretching Routine
Tight quadriceps pull the patella upward and increase pressure on the joint. The standing quad stretch, where you pull your heel toward your buttocks while keeping knees together, effectively targets this muscle group. Hold each stretch for 30 seconds and repeat 2-3 times per leg. Perform this stretch daily, especially after cycling.
The couch stretch, mentioned frequently by runners in online forums, addresses both the quadriceps and hip flexors simultaneously. Place one foot on a couch or bench behind you with the knee on the floor. Keep your torso upright and gently push your hips forward. This intense stretch should be held for 45-60 seconds per side.
Tight hamstrings limit knee extension and alter running mechanics. Lie on your back and loop a strap around your foot. Gently straighten your leg toward the ceiling until you feel a stretch in the back of your thigh. Hold for 30 seconds and repeat 2-3 times per leg. Keep the opposite leg flat on the floor for stability.
Calf tightness also affects knee mechanics. Perform the classic wall calf stretch with one leg forward and knee bent, back leg straight and heel down. Lean forward until you feel the stretch in your back calf. For the deeper soleus muscle, bend your back knee slightly while keeping the heel down. Hold each variation for 30 seconds.
Foam Rolling for IT Band and Surrounding Tissues
While you cannot directly roll the IT band itself (it is a thick fibrous tissue that does not respond like muscle), foam rolling the surrounding tissues provides significant benefit. Focus on the tensor fasciae latae (TFL) at the front of your hip, the vastus lateralis (outer quadriceps), and the gluteal muscles.
For the TFL, lie face-down with the foam roller positioned at the front of your hip, just below the bony prominence. Roll slowly side to side and up and down, pausing on tender spots for 20-30 seconds. This area often holds significant tension that contributes to lateral knee stress.
Roll the outer quadriceps by lying on your side with the roller positioned at the midpoint of your thigh. Move slowly from hip to knee, spending extra time on any tight or painful areas. The pressure should be firm but not excruciating. Breathe normally throughout the rolling session.
Perform foam rolling for 5-10 minutes daily, ideally before your stretching routine. The myofascial release prepares your tissues for stretching and helps break up adhesions that restrict normal movement. Consistency matters more than intensity.
Runner’s Knee Recovery Timeline
Most cases of runner’s knee resolve within 4 to 6 weeks with proper treatment. However, the exact timeline varies based on severity, adherence to the rehabilitation protocol, and whether you continue aggravating activities. Understanding the typical progression helps set realistic expectations and prevents the common mistake of returning too quickly.
During weeks 1-2, focus entirely on symptom reduction. This means strict adherence to RICE, elimination of painful activities, and beginning gentle strengthening exercises. Your knee should gradually become less painful during daily activities. If pain is not improving within a week, consider consulting a healthcare provider.
Weeks 3-4 involve progressive loading. As daily pain subsides, gradually introduce low-impact cardio like swimming and stationary cycling with low resistance. Continue your strengthening routine, progressing exercises as they become easier. Some athletes can begin walk-jog intervals during this phase if pain remains minimal.
Weeks 5-6 mark the return to running phase for most athletes. Start with short runs on flat terrain, avoiding hills and speed work initially. Monitor pain levels during and after runs. Mild discomfort that resolves within 24 hours is acceptable, but pain that lingers or worsens indicates you have progressed too quickly.
The key milestones that indicate readiness to progress include walking briskly without pain, performing 20 single-leg squats with good form and no pain, and completing your strengthening exercises without discomfort. Meeting these criteria before advancing your training reduces the risk of setbacks.
Triathlon-Specific Considerations
Triathletes face unique challenges when managing runner’s knee because they cannot simply stop all training. The goal is to modify rather than eliminate activity, maintaining fitness in two disciplines while allowing the knee to recover from the third. Here are the specific strategies that work for multisport athletes.
Bike Fit Adjustments
Optimizing your bike fit can significantly reduce patellofemoral stress. Start with saddle height. If your hips rock side to side at the bottom of the pedal stroke, your seat is too high. If your knees stay excessively bent throughout the stroke, it may be too low. Small adjustments of 2-3 millimeters can make a noticeable difference.
Saddle position fore-aft also matters. A saddle that is too far forward increases knee flexion angles and patellofemoral compression. When your crank is at 3 o’clock position, your knee should be directly over or slightly behind the pedal spindle. Professional bike fits typically address this, but many athletes never had a formal fit.
Cleat position influences knee tracking. For runners with knee issues, a slightly more rearward cleat position reduces the leverage forces on the knee during the pedal stroke. Ensure your cleats are properly aligned to prevent forced inward or outward knee deviation.
Transition Run Strategies
The bike-to-run transition is where many triathletes experience runner’s knee flare-ups. Start transition runs conservatively, allowing your legs to adjust to the new movement pattern. The first 5-10 minutes should be at a pace that feels almost embarrassingly easy. Your running form gradually normalizes as your muscles adapt.
Consider walking the first 30-60 seconds off the bike before starting your run. This brief walking period helps reset your muscle firing patterns and may reduce the initial shock loading on the knee. Some elite triathletes use this strategy specifically to protect their knees during heavy training blocks.
Swimming as Cross-Training
Swimming is the ideal cross-training activity during runner’s knee recovery. The water supports your body weight, eliminating impact stress while providing an excellent cardiovascular workout. Freestyle and backstroke keep the legs relatively straight, minimizing knee flexion. Avoid breaststroke, which involves significant knee bending and twisting motions that can aggravate PFPS.
Pool running with a flotation belt mimics running mechanics without the impact. This maintains your neuromuscular running patterns while protecting the knee. Many professional runners use deep water running during injury recovery to maintain fitness with zero ground reaction forces.
Training Through vs. Resting
The decision to train through runner’s knee or take complete rest depends on pain severity. A general rule is that pain level 3 or below on a 10-point scale during activity, which resolves completely within 24 hours, suggests you can continue modified training. Pain above this threshold or that lingers indicates you need more aggressive rest.
If you choose to train through, follow the 48-hour rule. Never perform back-to-back running days while recovering from runner’s knee. Alternate running with swimming or complete rest, and never run through pain that alters your gait. Limping creates compensations that lead to other injuries.
How to Prevent Runner’s Knee
Prevention is far easier than treatment. The strategies that help you recover from runner’s knee are the same ones that prevent it from recurring. Building these habits into your routine protects your knees through years of training and racing.
Follow the 10 percent rule for mileage progression. Never increase your weekly running volume by more than 10 percent from one week to the next. This applies to long runs, total weekly mileage, and intensity work. Triathletes must consider the combined load of all three disciplines, not just running.
Maintain year-round hip and glute strength. The exercises that fix runner’s knee also prevent it. Continue your clamshells, side leg lifts, and single-leg squats even after symptoms resolve. Two to three strength sessions per week provide the muscular foundation that protects your patellofemoral joint.
Prioritize proper warm-up before every run. Cold tissues are more susceptible to injury. A 5-10 minute dynamic warm-up that includes leg swings, walking lunges, and high knees prepares your muscles and joints for the demands of running. Never skip the warm-up, especially before hard workouts or races.
Rotate your running shoes and replace them regularly. Shoes lose their cushioning and support over time, typically after 300-500 miles. Running in worn-out shoes alters your mechanics and increases stress on the knees. Having multiple pairs in rotation allows each pair to fully decompress between runs.
Schedule regular gait analyses, especially after significant training changes or when you notice unusual wear patterns on your shoes. Small form corrections can prevent major problems. Many specialty running stores offer this service for free.
When to See a Doctor for Knee Pain
While most cases of runner’s knee respond to self-treatment, certain symptoms warrant professional evaluation. Recognizing these red flags prevents delayed diagnosis of more serious conditions and ensures appropriate care when home management is insufficient.
Seek medical attention if you experience any of the following: severe swelling that appears rapidly, inability to bear weight on the affected leg, locking or catching sensations in the knee, significant instability or giving way, fever accompanying knee pain, or pain that persists or worsens after 2-3 weeks of proper self-treatment.
A healthcare provider can rule out conditions like meniscus tears, ligament injuries, or arthritis that require different treatment approaches. They can also provide referrals to physical therapy for guided rehabilitation and assess whether imaging studies are appropriate.
Working with a sports medicine physician or physical therapist who understands endurance athletes is particularly valuable for triathletes. These providers can help modify your training to maintain fitness while addressing the underlying issues causing your pain.
Frequently Asked Questions
What is the fastest way to heal a runner’s knee?
The fastest way to heal runner’s knee is following the RICE protocol: Rest from aggravating activities, Ice for 15-20 minutes several times daily, Compression with a knee sleeve or strap, and Elevation above heart level. Combine this with daily strengthening exercises for hips and quadriceps, and you should see improvement within 1-2 weeks. Most cases resolve completely in 4-6 weeks with consistent treatment.
Can runner’s knee heal itself?
Yes, runner’s knee can heal itself with proper rest and activity modification. The body has remarkable healing capacity when given the right conditions. However, simply waiting without addressing the underlying muscle imbalances or training errors often leads to recurrence. Active rehabilitation through targeted exercises significantly improves healing speed and reduces the risk of the pain returning when you resume full training.
What triggers runner’s knee?
Runner’s knee is typically triggered by a combination of factors including sudden increases in training volume, downhill running or stairs, weak hip abductors and glutes that allow the knee to collapse inward, tight quadriceps and IT band pulling the patella off track, overpronation or biomechanical foot issues, and improper bike fit that forces the knee into excessive flexion. For triathletes, the transition from cycling to running is a common trigger due to pre-fatigued muscles and altered mechanics.
Does runner’s knee ever heal?
Yes, runner’s knee does heal completely in the vast majority of cases. Patellofemoral pain syndrome is rarely permanent when treated properly. Most athletes return to full activity within 4-6 weeks, though more severe or chronic cases may take 8-12 weeks. The key is addressing both the symptoms and the underlying causes. Without correcting muscle imbalances or training errors, the condition may become chronic or recur frequently.
Can a chiropractor fix runner’s knee?
A chiropractor can help with runner’s knee as part of a comprehensive treatment approach, particularly if joint alignment issues contribute to your symptoms. Chiropractic adjustments may improve pelvic and lower extremity alignment, reducing the mechanical stress on the patellofemoral joint. However, chiropractic care alone is rarely sufficient. It works best when combined with physical therapy exercises, training modifications, and proper footwear or orthotics if needed.
Is walking good for runner’s knee?
Walking is generally good for runner’s knee if it does not provoke pain. It maintains cardiovascular fitness and promotes blood flow to healing tissues without the impact forces of running. Start with flat surfaces and moderate paces, avoiding hills initially. If walking causes pain, switch to swimming or deep water running temporarily. As symptoms improve, gradually increase walking distance and introduce gentle hills before returning to running.
Conclusion
Runner’s knee is one of the most common yet manageable injuries facing triathletes and runners. Understanding what is runner’s knee and how to fix it empowers you to take control of your recovery and return to training stronger than before. The combination of proper rest, targeted strengthening, and smart training modifications has helped thousands of athletes overcome this condition without surgery or prolonged time off.
Remember that the exercises and strategies in this guide work best when applied consistently. Building hip strength, maintaining flexibility, and following gradual progression principles not only fix current knee pain but prevent future episodes. Your knees are built to last through years of swimming, cycling, and running when you give them the care they deserve.
Start your recovery protocol today, be patient with the healing process, and you will be crossing finish lines pain-free throughout 2026 and beyond.