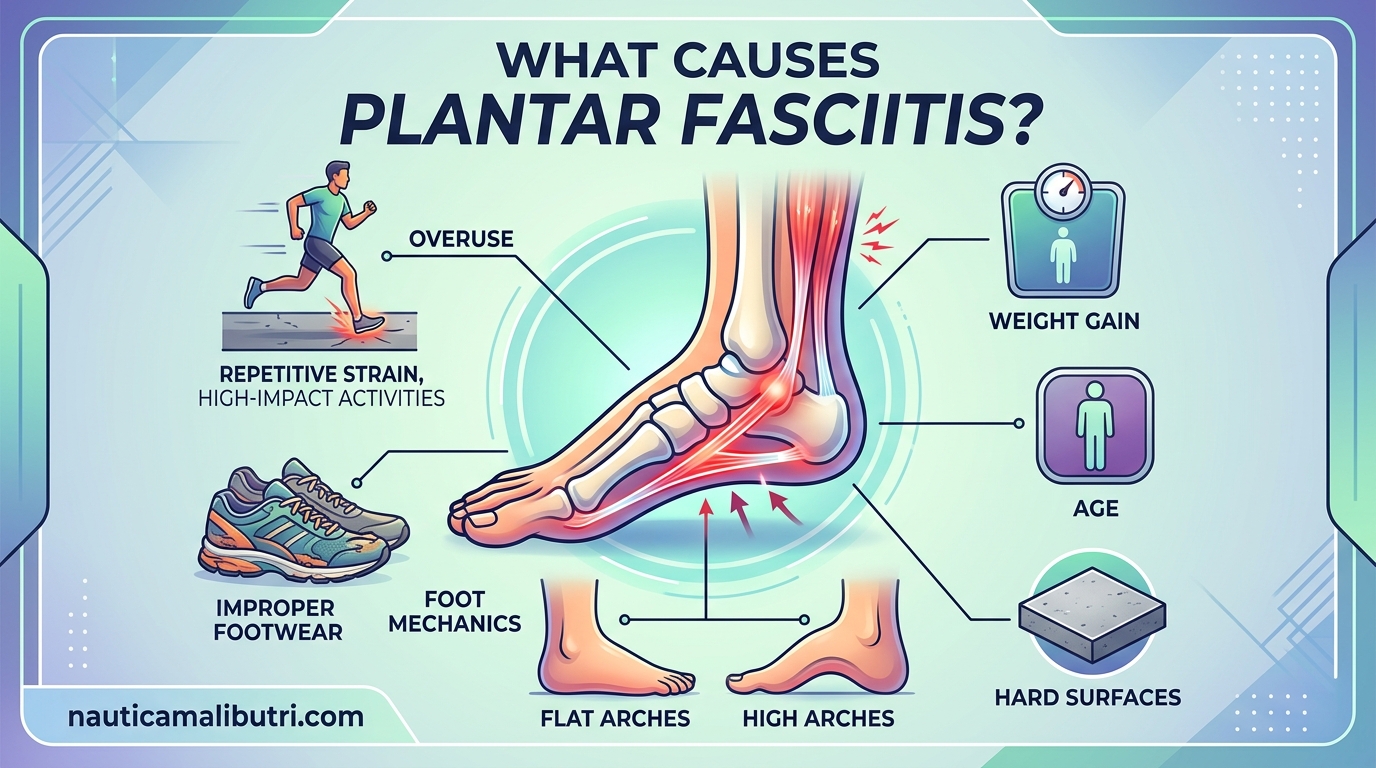
Nothing derails a training block quite like that first sharp step out of bed in the morning. If you are a triathlete or runner who has experienced that stabbing heel pain, you already know how debilitating plantar fasciitis can be. What causes plantar fasciitis is a question I hear constantly from athletes at the Nautica Malibu Triathlon and in training forums across the endurance community.
Plantar fasciitis affects approximately 1 in 10 people during their lifetime, with runners and athletes facing significantly higher risk. The condition develops when the thick band of tissue connecting your heel to your toes becomes irritated, inflamed, or degenerated from overuse. Understanding the root causes helps you prevent this setback and maintain consistent training throughout your race season.
This guide covers the primary causes, individual risk factors, and the triathlon-specific scenarios that can trigger plantar fasciitis. We will explore everything from basic biomechanics to the unique challenges of T2 transitions and brick workouts that multisport athletes face.
Table of Contents
What Is Plantar Fasciitis
Plantar fasciitis is an overuse injury affecting the plantar fascia, a thick fibrous band of tissue that runs along the bottom of your foot. This ligament connects your heel bone (calcaneus) to the base of your toes and supports the longitudinal arch of your foot during weight-bearing activities.
The plantar fascia acts like a shock-absorbing bowstring. When you walk, run, or jump, this tissue tightens to help maintain your arch and absorb impact forces. Under normal conditions, the fascia can handle significant stress. Problems develop when repetitive strain exceeds the tissue’s capacity to repair itself.
Contrary to popular belief, plantar fasciitis is not purely an inflammatory condition. Research now shows it involves micro tears, collagen degeneration, and tissue breakdown rather than simple inflammation. This explains why traditional anti-inflammatory treatments alone often fail to resolve the issue.
The hallmark symptom is sharp heel pain, particularly with the first steps after waking or after prolonged sitting. Many triathletes report that the pain improves during activity but returns with a vengeance afterward. Understanding what causes plantar fasciitis requires examining both mechanical stressors and individual susceptibility factors.
What Causes Plantar Fasciitis
The primary driver of plantar fasciitis is excessive strain on the plantar fascia beyond what it can adapt to and repair. This strain comes from repetitive loading, biomechanical inefficiencies, and training errors that accumulate over time. Let us break down the major categories.
Overuse and Repetitive Stress
Excessive training volume represents the most common cause among endurance athletes. The plantar fascia tolerates daily stress remarkably well until the cumulative load exceeds tissue capacity. Runners increasing weekly mileage by more than 10 percent per week face significantly elevated risk.
Micro tears develop in the fascia tissue when impact forces become too frequent or too intense. Unlike muscles that adapt quickly to stress, connective tissue requires longer recovery periods. Athletes who run every day without adequate rest between sessions create an environment where damage outpaces repair.
Training intensity spikes also contribute significantly. Adding speed work, hill repeats, or tempo runs too quickly changes the loading patterns on your feet. Downhill running is particularly problematic because it increases braking forces and extends the foot’s contact time with the ground.
Biomechanical Factors
How your foot strikes the ground and moves through the gait cycle profoundly affects plantar fascia stress. Overpronation, where the foot rolls excessively inward after heel strike, stretches and strains the plantar fascia with each step. This abnormal motion increases tension on the medial band of the tissue.
Supination, or underpronation, creates different problems. High-arched feet that do not pronate enough fail to absorb shock effectively. This transfers more impact force directly to the heel and plantar fascia. Both extremes of foot motion increase tissue stress beyond healthy levels.
Gait abnormalities including leg length discrepancies, tibial rotation issues, and hip weakness can alter foot mechanics. When upstream structures fail to stabilize properly, the foot compensates by changing its strike pattern. These compensations often overload the plantar fascia.
The Heel Pain Connection
Understanding morning pain helps explain the underlying mechanism. During sleep, your foot naturally points downward, shortening the plantar fascia and Achilles tendon. Upon waking, those first steps suddenly stretch the tissue that has tightened overnight. This rapid elongation of a stiff, damaged structure produces that characteristic stabbing sensation.
The pain pattern offers diagnostic clues. If your heel hurts most with the first few steps but improves as you move, classic plantar fasciitis is likely. Pain that worsens throughout the day suggests other conditions. This distinction matters for proper treatment selection.
Risk Factors That Increase Your Chances
While anyone can develop plantar fasciitis, certain characteristics significantly increase susceptibility. These factors interact with training stress to create the perfect storm for tissue damage. Understanding your individual risk profile helps you take preventive action before problems develop.
Foot Structure and Arch Type
Foot architecture plays a major role in plantar fascia loading. Flat feet (pes planus) allow the arch to collapse excessively during weight bearing. This stretching motion elongates the plantar fascia beyond its comfortable range with every step. Athletes with fallen arches often benefit significantly from arch support.
High arches (pes cavus) create the opposite problem. The rigid foot structure fails to absorb shock properly, concentrating impact forces on the heel and forefoot. These athletes experience more direct trauma to the plantar fascia insertion point at the calcaneus.
Both foot types can function well with appropriate footwear and conditioning. The issue arises when athletes with structural variations train hard without addressing their specific biomechanical needs. Proper shoe selection becomes especially important for these individuals.
Body Weight and Load
Excess body weight increases plantar fascia strain with every step. Research shows that individuals with BMI over 30 face three times the risk of developing plantar fasciitis. Even modest weight gain of 15 pounds can trigger symptoms in susceptible athletes.
Pregnancy represents a unique risk period. Hormonal changes loosen ligaments throughout the body, including the plantar fascia. Combined with the rapid weight gain of pregnancy, this creates temporary vulnerability that may persist postpartum if not addressed.
For triathletes, the impact is less about absolute weight and more about the repetitive loading pattern. A heavier runner who lands softly with good mechanics may experience less tissue stress than a lighter runner with poor form. Nevertheless, maintaining healthy body composition reduces overall risk.
Age and Tissue Changes
Plantar fasciitis most commonly affects adults between 40 and 60 years old. This age distribution reflects natural changes in tissue quality. Collagen fibers become less elastic and more prone to micro damage as we age.
Blood supply to the plantar fascia also decreases over time. Reduced perfusion means slower healing and less capacity to adapt to training stress. Older athletes need longer recovery periods between hard sessions to allow tissue repair.
However, age alone does not doom you to injury. Masters athletes who respect recovery needs and maintain flexibility often outperform younger athletes who ignore warning signs. The key is adapting training volume and intensity to match your tissue capacity at any age.
The Role of Tight Muscles and Tendons
Tightness in the posterior chain creates a cascade of mechanical problems that often manifests as plantar fasciitis. The gastrocnemius and soleus muscles connect to the Achilles tendon, which in turn blends into the plantar fascia. Tension anywhere along this chain increases stress on the heel attachment.
The gastrocnemius muscle crosses both the knee and ankle joints. When tight, it limits ankle dorsiflexion, preventing the tibia from moving forward properly over the foot during gait. This restriction forces the foot to compensate by increasing pronation or altering strike mechanics.
The Achilles tendon shares fascial connections with the plantar fascia. Tightness here directly transfers tension to the heel bone insertion. Athletes with limited ankle flexibility often develop heel pain even when their training load seems reasonable. Addressing calf tightness frequently resolves stubborn plantar fasciitis cases.
Stretching protocols that target both the gastrocnemius (with knee straight) and soleus (with knee bent) provide comprehensive coverage. Foam rolling and massage can supplement static stretching to address tissue adhesions. Consistency matters more than intensity with flexibility work.
Triathlon-Specific Causes
Triathletes face unique challenges that pure runners often avoid. The combination of three disciplines creates specific mechanical and training stressors that increase plantar fasciitis risk. Understanding these multisport factors helps you modify training to stay healthy.
The T2 Transition Problem
The transition from bike to run (T2) creates one of the most abrupt biomechanical shifts in endurance sports. Cycling locks your foot in a fixed position with minimal ankle movement for extended periods. Blood pools in the feet from the sustained pressure of pedaling. Then you suddenly demand full weight-bearing range of motion from stiff, slightly swollen feet.
Many triathletes report their worst plantar fasciitis pain during the first mile off the bike. The pre-fatigued calf muscles and Achilles tendon cannot absorb impact forces normally. This creates a spike in plantar fascia stress precisely when the tissue is least prepared to handle it.
Adding short run segments immediately after bike training sessions helps your feet adapt to the transition. Even five minutes of easy jogging after a long ride prepares the tissue for race-day demands. Neglecting this specific preparation leaves you vulnerable on race morning.
Brick Workouts and Fatigue
Brick workouts serve an essential purpose in triathlon preparation, but they also stress the plantar fascia uniquely. Running on pre-fatigued legs alters your gait mechanics significantly. Stride length typically shortens, cadence increases, and ground contact time changes. These alterations modify how force transfers through your feet.
Form breakdown during the run portion of bricks often includes increased heel striking and reduced knee flexion. Both patterns increase shock transmission to the plantar fascia. The tissue must absorb forces that larger muscle groups normally handle when fresh.
Modulating brick workout frequency and intensity helps manage this risk. Not every brick needs to be a hard session. Easy bike-to-run transitions build the specific adaptation without overwhelming tissue repair capacity.
Pool Deck Walking
Triathletes spend significant time walking barefoot on pool decks, in locker rooms, and around transition areas. Hard concrete surfaces offer no shock absorption whatsoever. Walking barefoot removes the support and cushioning that quality footwear provides.
The combination of wet feet and hard surfaces is particularly problematic. Wet skin softens and provides less natural protection. Concrete pool decks transmit nearly all impact force directly to your feet without the attenuation that occurs on softer surfaces.
Wearing slide sandals or flip flops with arch support around the pool deck protects your feet during the significant time spent on these surfaces. Saving your barefoot time for the pool itself, not the surrounding concrete, reduces cumulative stress.
Build Phase Volume Spikes
Triathlon training naturally includes significant volume increases during build phases. The progression from base training to race-specific preparation often involves simultaneous increases in swimming, cycling, and running. While running mileage might increase modestly, the total training stress spikes dramatically.
This cumulative fatigue affects tissue recovery even when individual sessions seem manageable. The plantar fascia repairs itself during rest periods between training stimuli. When three-sport training fills nearly all available time, repair windows shrink.
Monitoring total training stress rather than just running mileage helps prevent overload. Tools like Training Stress Score (TSS) or subjective fatigue ratings capture the multisport load that running logs miss. Respecting recovery becomes even more important when training three disciplines.
Activity and Footwear Contributors
Beyond training volume and biomechanics, specific activities and shoe choices significantly influence plantar fasciitis development. These factors are often within your direct control, making them prime targets for prevention strategies.
Training Surfaces That Cause Problems
Hard surfaces increase impact forces transmitted through the plantar fascia. Concrete provides essentially no shock absorption, transferring all energy back into your body. Asphalt offers slightly more give, while trails and tracks provide the most cushioning.
However, soft surfaces are not automatically safer. Very soft sand or mud changes foot mechanics and can increase strain on the plantar fascia as your foot works harder to push off. The key is variety rather than seeking the softest possible surface exclusively.
Downhill running deserves special mention. The braking forces required to control descent place unique stress on the plantar fascia. The foot lands with the toes higher than the heel, pre-stretching the tissue before impact. Downhill sections in races often trigger acute flare-ups.
Footwear Mistakes
Worn-out running shoes lose their shock absorption capacity long before they look damaged. Midsole foam compresses gradually, reducing cushioning without visible external signs. Most running shoes require replacement after 300 to 500 miles depending on your weight and running mechanics.
Inadequate arch support allows excessive pronation in susceptible runners. While some athletes function well in neutral shoes, others need structured footwear to control foot motion. Matching shoe type to your specific foot mechanics prevents unnecessary tissue stress.
Flip flops and unsupportive casual shoes contribute to plantar fasciitis even when you are not training. Time spent walking around in flat, unsupportive footwear accumulates stress on the plantar fascia. Recovery footwear with arch support helps the tissue rest between training sessions.
The minimalist shoe transition trend caused problems for many runners. Abruptly switching to zero-drop, minimally cushioned shoes changes loading patterns dramatically. Gradual transition periods of several months allow tissue adaptation. Rushing the process frequently results in plantar fascia damage.
Frequently Asked Questions
What is the major cause of plantar fasciitis
The major cause of plantar fasciitis is overuse and repetitive stress on the plantar fascia beyond its capacity to repair. This typically occurs from sudden increases in training volume, excessive standing on hard surfaces, or biomechanical factors that concentrate stress on the heel attachment. For triathletes, the combination of running, cycling position, and pool deck walking creates unique cumulative stress that increases risk.
What is the root cause of plantar fasciitis
The root cause involves collagen degeneration and micro tears in the plantar fascia tissue rather than simple inflammation. When repetitive strain exceeds the tissue’s repair capacity, the fascia develops degenerative changes at the heel bone insertion. Contributing factors include tight calf muscles, abnormal foot mechanics, inadequate recovery between training sessions, and hard training surfaces that increase impact forces.
Why did I suddenly develop plantar fasciitis
Sudden onset of plantar fasciitis usually follows a specific trigger event combined with underlying susceptibility. Common triggers include a rapid training volume increase, switching to new shoes with different support characteristics, gaining weight, or starting a job that requires prolonged standing. The tissue was likely approaching its tolerance limit before the triggering event pushed it over the threshold into symptomatic territory.
Can running cause plantar fasciitis
Running can cause plantar fasciitis when training volume increases too quickly or when biomechanical factors concentrate stress on the heel. However, running itself is not inherently damaging when approached progressively. Most cases result from training errors like increasing weekly mileage by more than 10 percent, inadequate recovery between hard sessions, or running on hard surfaces without proper footwear.
Does plantar fasciitis fully recover
Most cases of plantar fasciitis do fully recover with appropriate treatment, though the timeline varies significantly. Approximately 90 percent of patients improve within 6 to 12 months using conservative treatments like stretching, orthotics, and activity modification. However, without addressing underlying causes like training errors, biomechanical issues, or footwear problems, recurrence is common when activity resumes.
Can tight calves cause plantar fasciitis
Tight calf muscles are a significant contributing factor to plantar fasciitis. The gastrocnemius and soleus muscles connect through the Achilles tendon to the plantar fascia. When these muscles lack flexibility, they restrict ankle dorsiflexion and increase tension on the plantar fascia during gait. Addressing calf tightness through consistent stretching and foam rolling often resolves stubborn plantar fasciitis cases that do not respond to other treatments.
Why does plantar fasciitis hurt more in the morning
Morning pain occurs because the plantar fascia and Achilles tendon naturally tighten while you sleep with your feet pointed downward. The first steps after waking suddenly stretch this shortened tissue, creating sharp pain at the heel insertion. As you move and warm up the tissue, flexibility improves and pain typically decreases. Night splints that maintain gentle stretch can reduce morning symptoms significantly.
Can flat feet cause plantar fasciitis
Flat feet (pes planus) increase plantar fasciitis risk by allowing the arch to collapse excessively during weight bearing. This stretching motion elongates the plantar fascia beyond its comfortable range with each step. However, flat feet alone do not guarantee injury. Many athletes with flat feet train injury-free by using appropriate arch support and maintaining strong intrinsic foot muscles that help control arch collapse.
Conclusion
Understanding what causes plantar fasciitis empowers you to prevent this common overuse injury from derailing your training. The condition develops when repetitive stress exceeds your plantar fascia’s capacity to repair itself. Primary drivers include overuse, biomechanical inefficiencies, tight calf muscles, and hard training surfaces.
Triathletes face additional risk factors unique to multisport training. T2 transitions, brick workouts, pool deck walking, and build phase volume spikes all contribute to cumulative foot stress. Addressing these specific challenges helps you maintain consistent training throughout your race season.
Most cases of plantar fasciitis resolve with conservative treatment when addressed early. Do not ignore that morning heel stiffness hoping it will disappear. Identifying and modifying the specific causes in your training, footwear, and biomechanics puts you back on track toward your 2026 racing goals.